
Repigmentation rates have been reported to be between 41.6% and 100%. Phototherapy may increase the incidence of both melanoma and non-melanoma skin cancer, and cumulative lifetime dose should be capped at 500 treatments. This modality works both as an immunosuppressive and through direct stimulation of melanocyte proliferation. Phototherapy is used as a third line treatment for patients who fail combination topical therapy. 
This product is safe to use in both children and adults, with the best response seen in combination with topical steroids. Common side effects are erythema, pruritus, burning and irritation.Ĭalcipotriene is a topical vitamin D3 analog and is used as an equal second-line treatment for patients who fail topical corticosteroid therapy. They are both safe for short term or intermittent long-term use. They do not produce epidermal atrophy, folliculitis, telangiectasia or the striae that may be associated with topical corticosteroid use. Topical calcineurin inhibitors (tacrolimus and pimecrolimus) which are immunomodulators, are used as a second-line treatment for patients who fail topical corticosteroid therapy. Oral prednisolone, pulse intravenous methylprednisolone and pulse intravenous dexamethasone have all been used. Systemic corticosteroids can halt disease progression and induce repigmentation in patients with rapidly progressive vitiligo. Systemic absorption can lead to adrenocortical suppression when large areas of vitiligo are being treated with topical corticosteroids. Potential local side effects from topical corticosteroids include epidermal atrophy, folliculitis, telangiectasia and striae. The highest response rates are seen in children with head and neck lesions. 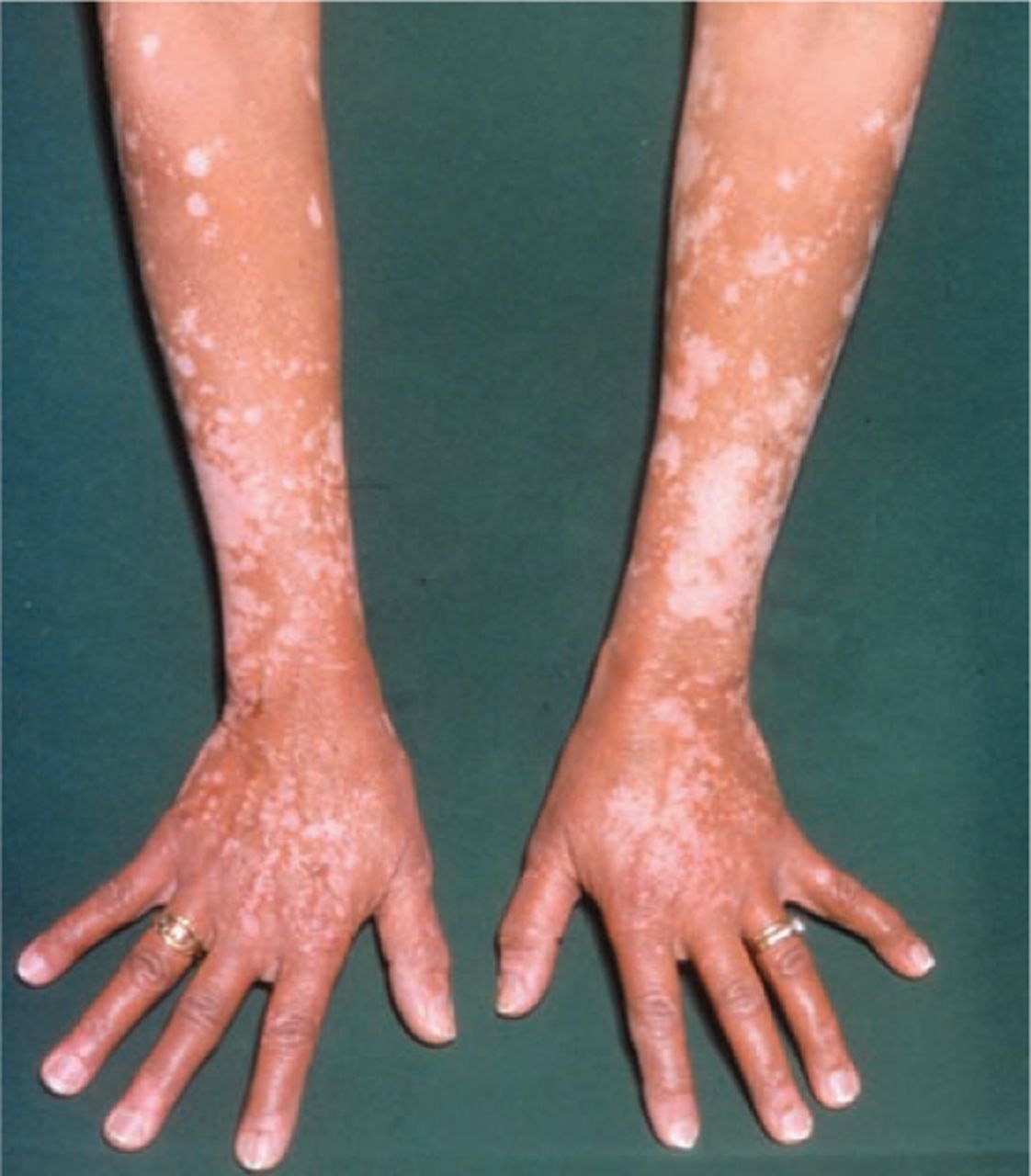
Topical steroids have been studied in both adults and children. Treatment should be continued for at least three months before being deemed to have failed. Topical steroids are preferred for stable or slowly progressing vitiligo, while systemic steroids are reserved for active, rapidly extending disease. Treatments may be directed at depigmentation of unaffected skin for patients with extensive or recalcitrant disease, where repigmentation or camouflage creams to conceal affected skin is not feasible.Ĭorticosteroids are used as first line treatment for vitiligo. Oral therapy is reserved for rapidly extending vitiligo. Nevertheless, most patients can achieve partial or complete repigmentation of individual lesions with topical treatment, phototherapy or surgery. In the absence of gene therapy, there is no cure. This is the most common clinical subtype. Generalised vitiligo may begin in later life, at sites of pressure, friction or trauma and is usually progressive with flare-ups.Segmental vitiligo produces unilateral maculae in a band‐shaped distribution. Segmental vitiligo typically begins in childhood, occurring most commonly in the trigeminal dermatome, with poliosis (an absence or decrease of melanin in the hair, eyelashes, eyebrows or any other hairy area), and tends to be stable. Localised vitiligo which is further subdivided into focal, segmental and mucosal.Vitiligo is divided into two clinical sub-types: Without treatment, vitiligo tends to progress, although spontaneous repigmentation may occur occasionally. Severe sunburn, pregnancy and emotional stress may precede the onset. Vitiligo commonly occurs at sites that are normally hyperpigmented - including the face (periorificial), dorsal surfaces of hands, nipples, axillae, umbilicus, sacrum and inguinal regions. There is no surface change noted in vitiliginous skin. The macules and patches of vitiligo are discrete, and uniformly white with convex borders surrounded by normal skin. The rate of progression is variable it may extend rapidly over a period of several months and then remain quiescent for many years. The macules gradually enlarge, and new lesions appear progressively. In vitiligo, selective destruction of epidermal melanocytes produces well-circumscribed depigmented macules of the skin and mucous membranes. Some 30-40% of patients have a positive family history and the onset is often earlier in this cohort. The condition can begin at any age, but 50% of cases develop before the age of 20. It occurs in all ethnicities and skin types and is equally prevalent in men and women. Vitiligo affects approximately 1% of the world’s population however, estimates of prevalence range from less than 0.1% to greater than 8%.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
